Overview
Scoliosis means a curve in the spine. If your child has a condition that causes problems with the muscles or with their brain, spinal cord, or nerves, then your child can develop a type of scoliosis known as neuromuscular scoliosis.Conditions that can cause neuromuscular scoliosis can be divided into two groups, those that affect the brain/spinal cord/nerves or those that mainly affect the muscles:
| Brain, Spinal Cord, or Nerves Affected | Muscles Affected |
| Cerebral palsy (CP) | Arthrogryposis |
| Friedreich ataxia | Muscular dystrophy |
| Charcot-Marie-Tooth disease | Congenital myopathy |
| Roussy-Levy disease | Fiber-type disproportion |
| Syringomelia | Congenital hypotonia |
| Spinal cord tumors | Myotonia dystrophica |
| Spinal cord trauma/injury | |
| Rett syndrome | |
| Poliomyelitis | |
| Spinal muscular atrophy (SMA) | |
| Dysautonomia | |
| Spina bifida / Myelomeningocele |
If your child has one of these conditions, they may develop a curvature of their spine due to nerve and/or muscle imbalance.
Symptoms
When looking at your child from behind, the curve in the spine may make one shoulder higher than the other, or their waist may look straight on one side and more curved on the other, and the ribs may be higher on one side as seen in Figure 1A. If the pediatric orthopaedic surgeon takes an X-ray of your child’s spine, they may see a “C-shaped” curve as seen in Figure 1B. Sometimes your child’s back may be “S-shaped”, or it may be more curved looking from the side than from the back. This is called “kyphosis” and if your child develops this, it may also cause issues. In a child who spends most of their time in a wheelchair, these curves may cause issues with sitting and comfort. Most children, however, do not have pain from their spinal curvatures. You will be asked about any concerns you have at each appointment.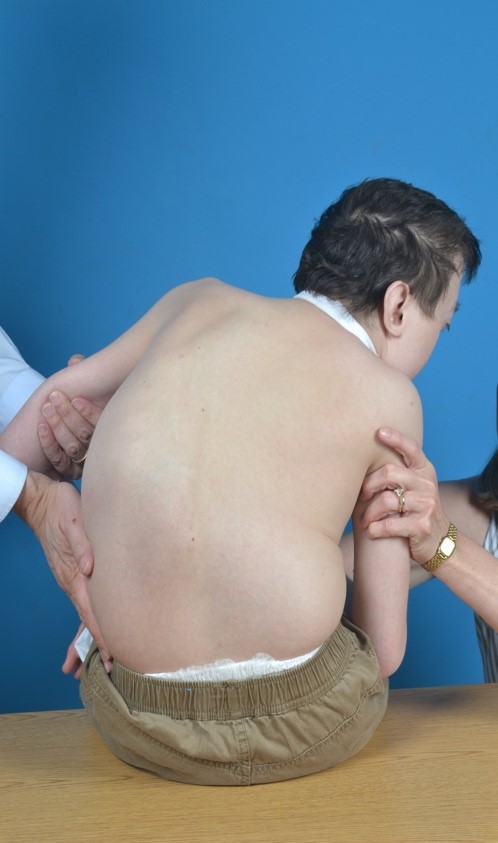
Figure 1A - How your child’s back my look from behind due to their curve.
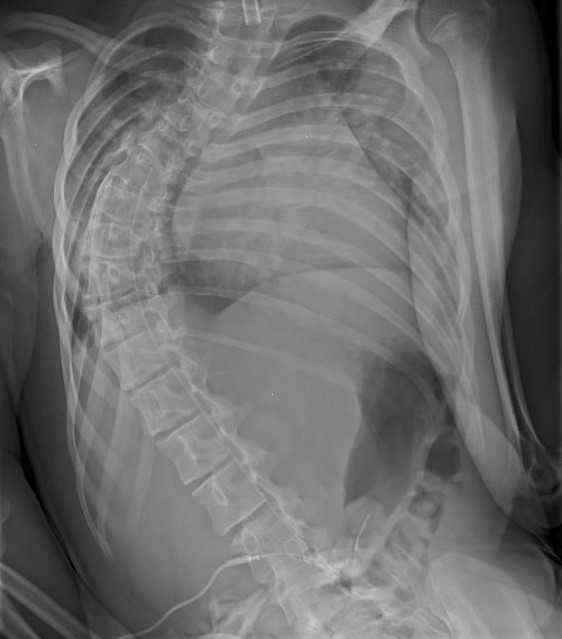
Figure 1B - An x-ray that shows what type of “C-shaped” curve may cause your child’s back to look abnormal
Examination & Evaluation
If your child has a neuromuscular condition – he or she will have multiple providers seeing them routinely. One of those doctors may be a pediatric orthopedic surgeon. That doctor will want to know all about your child’s birth and diagnosis as well as other problems and other doctors they see. The doctor will look at your child’s back to examine the skin and assess the shoulders. The examination will involve standing and bending unless your child does not stand, in which case your child will be looked at on the examination table and in their chair. Your doctor may test your child’s nerves looking for weakness or numbness. They may evaluate your child lying down to see how flexible the scoliosis is.Any child with a neuromuscular diagnosis should be checked for scoliosis because curves are very common. Your orthopaedic surgeon may get X-rays periodically, however getting an X-ray at every visit is not always needed. Depending on the neuromuscular diagnosis, there are other tests that your child may need including a CT scan and an MRI of the spine.
Treatment
Bracing - Bracing has not been shown to improve scoliosis or prevent it from getting worse in children with neuromuscular diseases. If a brace is used, it is usually used to improve how your child sits in their wheelchair. Bracing has also been used to try and slow the progression of a curve to safely delay any future surgery. The trunk bolsters and hip pads in a wheelchair can also be used to help correct your child’s spine while sitting and aid in transport/comfort and improve overall quality of life.Surgery - If your child’s curve has a major effect on their quality of life, breathing, or ability to eat, then your surgeon may recommend surgery. It is usually difficult to know how much the scoliosis is bothering children in cases where they are not able to speak. Surgery involves taking your child’s curved spine (Figure 2A), and inserting rods and screws to decrease your child’s curve to a safe level and balance their seating position (Figure 2B). The entire surgery is called “spinal fusion” because it makes the separate bones in your child’s spine join together. To help improve your child’s sitting, the fusion may require adding screws into their pelvis. The surgery is complex, and has a lot of risks. Your doctor will spend time with you discussing the risks and benefits of surgery so you can make the best decision for your child. Surgery is never absolutely required, but may be recommended to help improve your child’s quality of life.
In young children (age less than 8-10) your surgeon may use rods that grow with your child until your child reaches an age where they can have a permanent spinal fusion.



 POSNA.org
POSNA.org