POSNA.org
POSNA.org
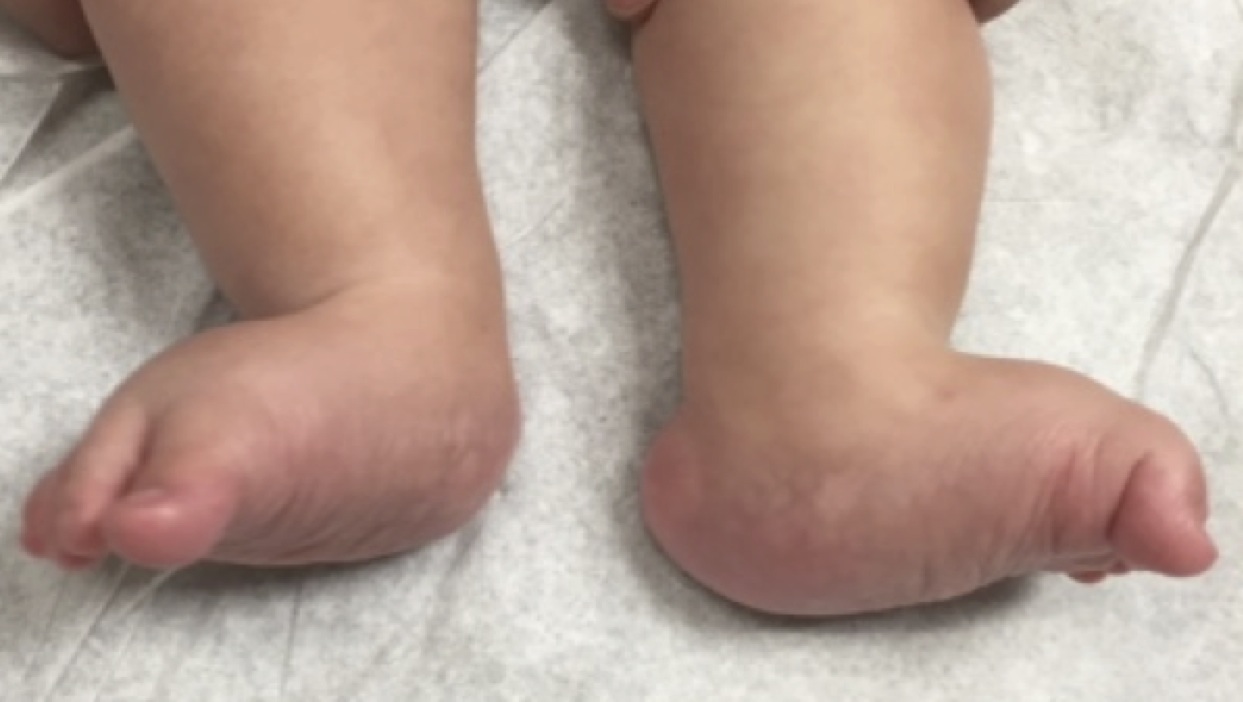
Vertical talus is usually noted at birth; however, it can sometimes be detected on ultrasound during pregnancy. Examination of the foot is important. Your doctor will try to feel the bones in the foot and manipulate the foot to see if the deformity is flexible or rigid. Some children will be walking age or even older and have one or both feet appear very flat when standing.
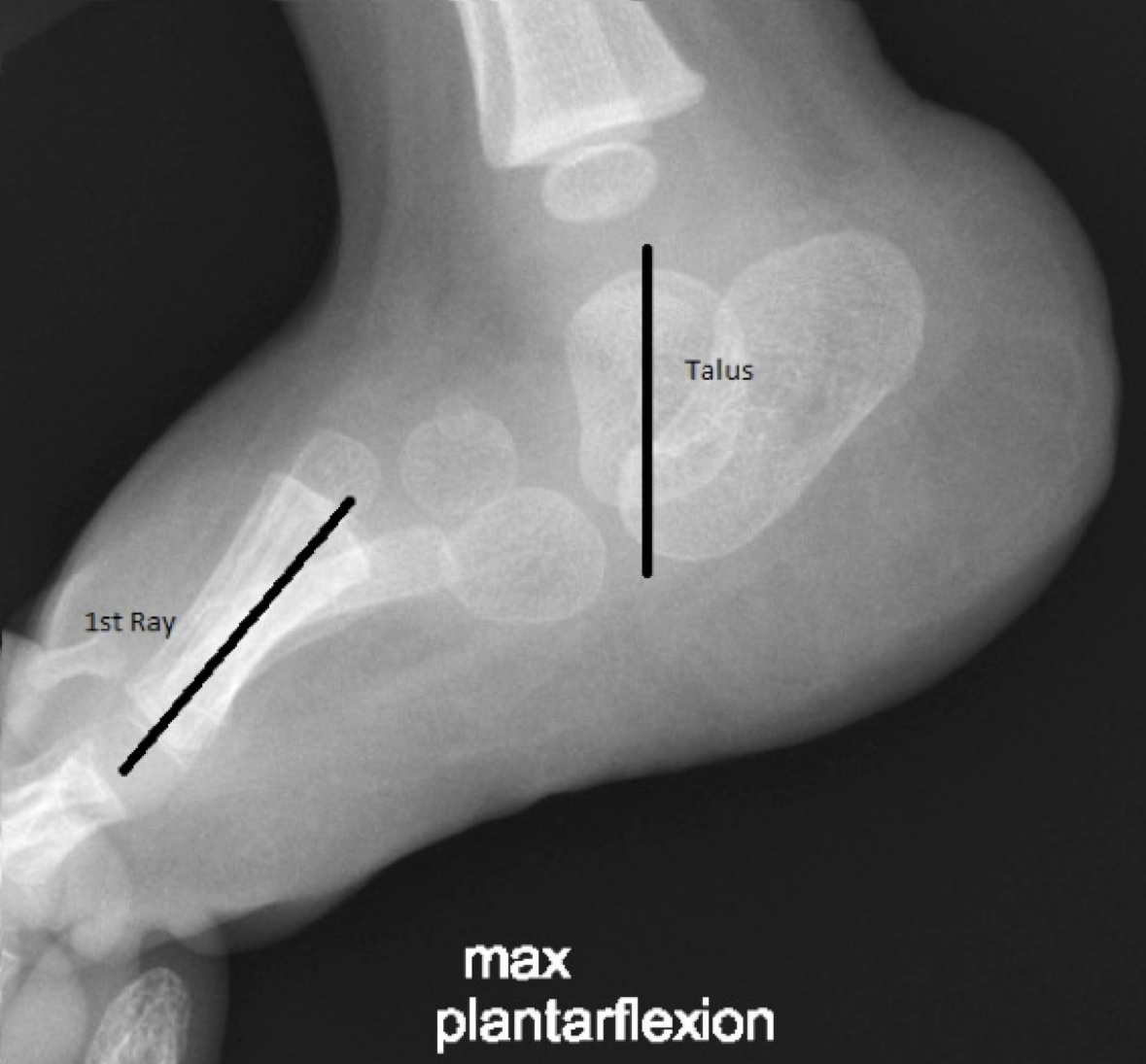
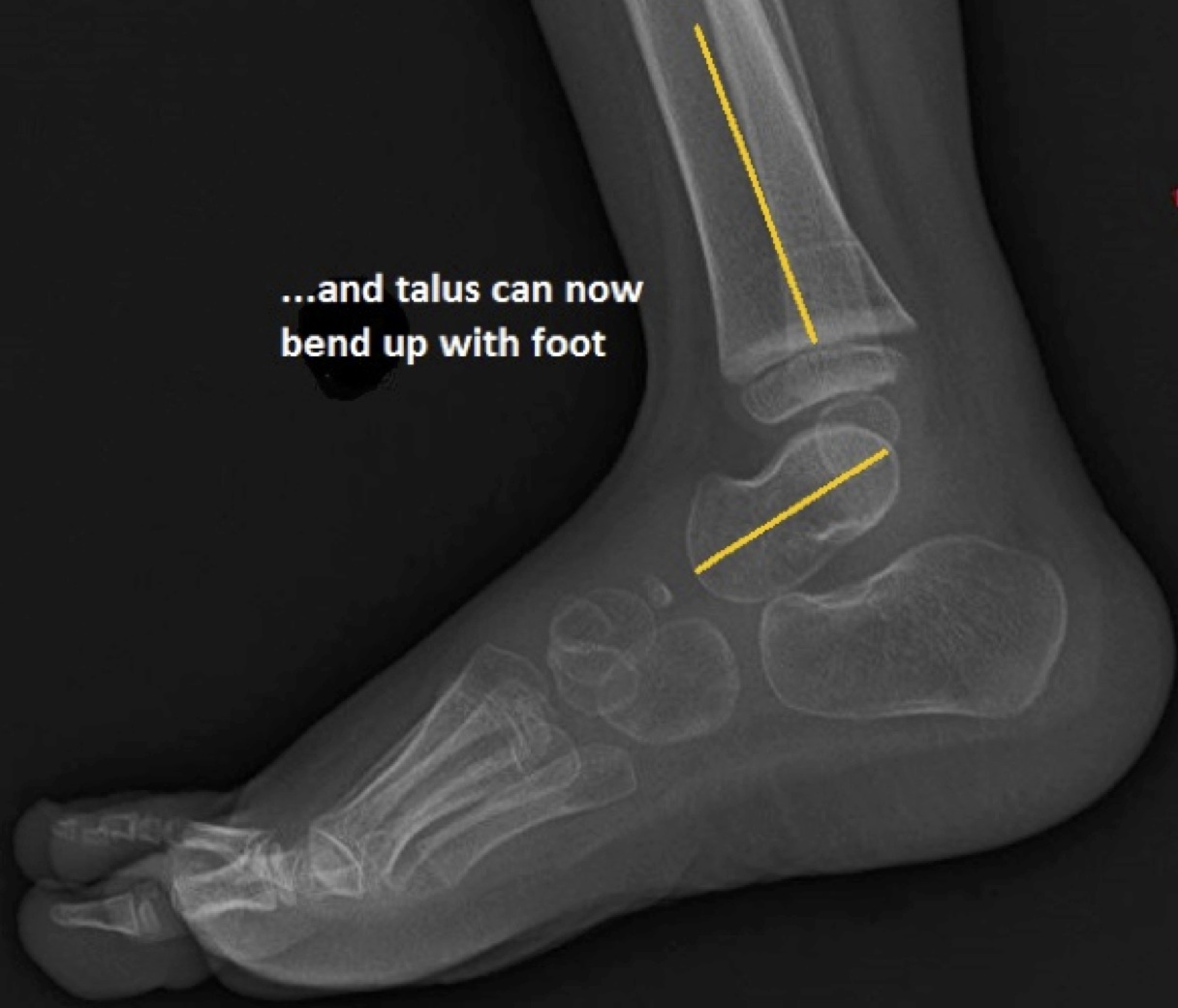
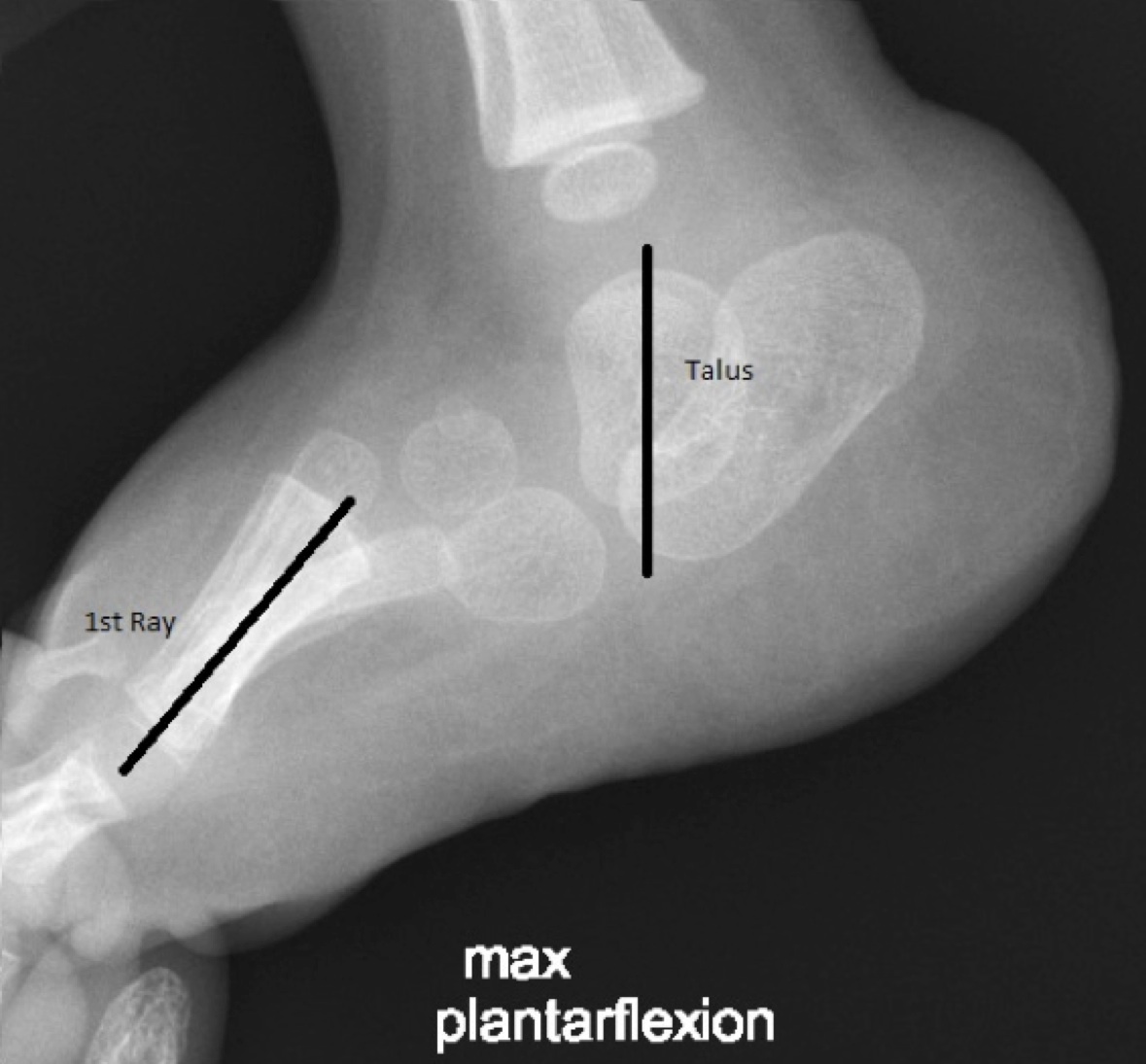
Your doctor will probably order an x-ray. In particular, an x-ray with the foot pointing downward (referred to as plantarflexion) can help determine if the bones in front of the talus line up properly or are stuck on top of the talus.
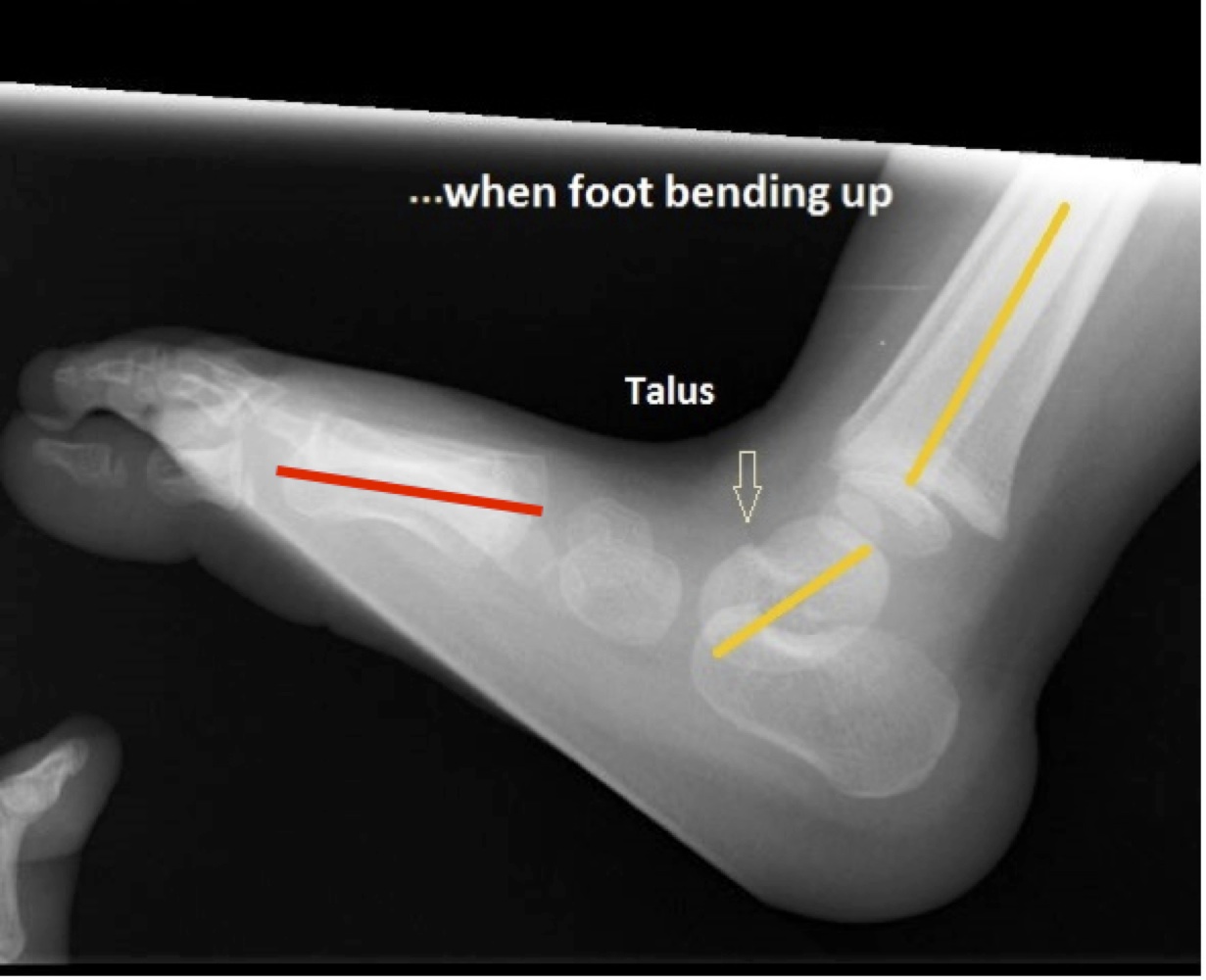
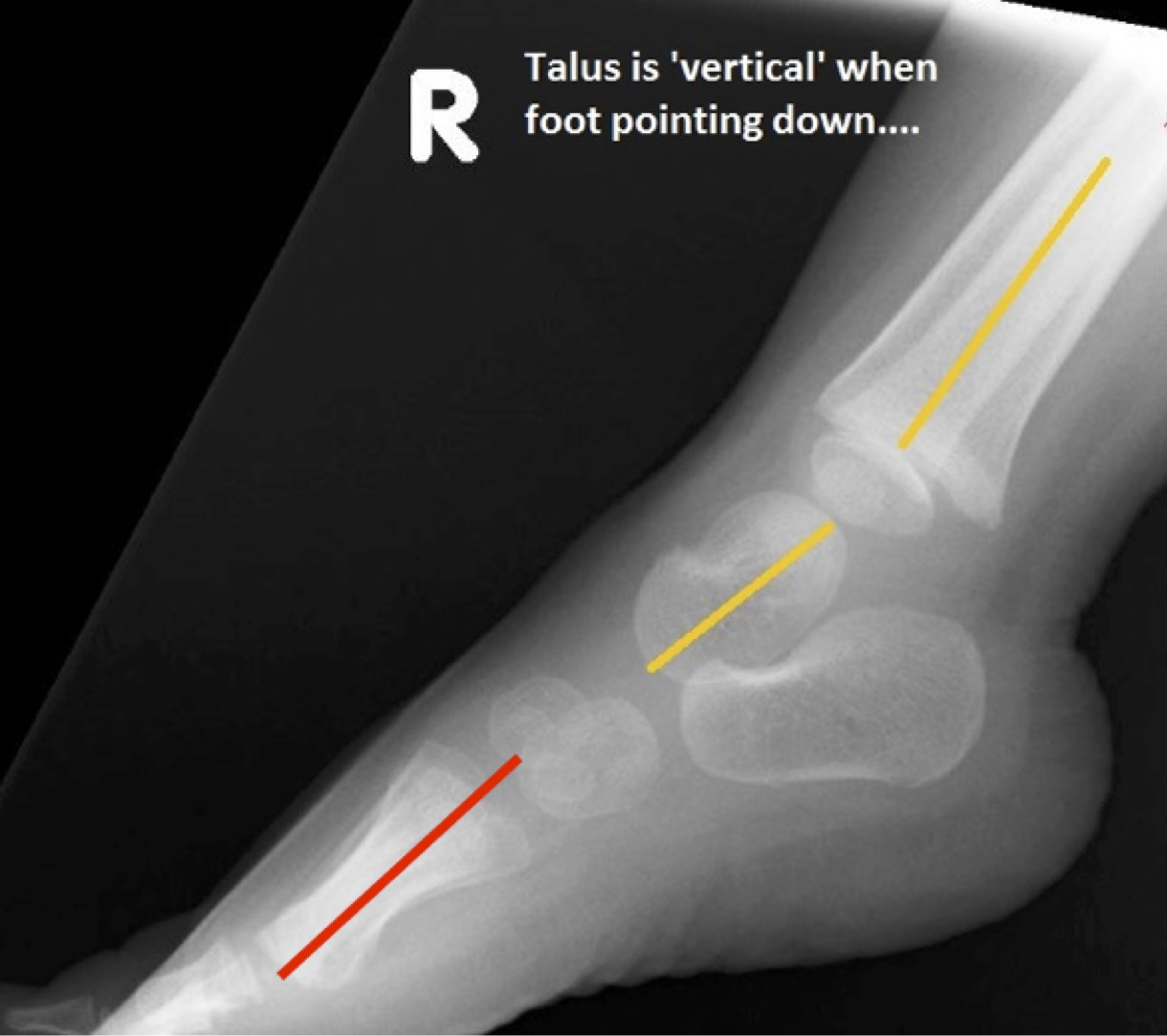
Vertical talus should be treated with the goal of providing a painless, stable, functional foot that fits in shoes comfortably. Initially, vertical talus is not painful. If left untreated, however, the foot will remain deformed and eventually become painful as the child begins to walk and increase activity. Calluses or skin breakdown can occur in the flattened arch area, making it difficult to wear shoes and walk.
Some surgery is usually needed to correct the vertical talus deformity. Before surgery, however, your doctor may recommend a trial of stretching or casting to improve the flexibility of the foot. This may decrease the amount of surgery that is needed, or, in some cases, prevent the need for surgery all together. Casting usually requires multiple visits to your doctor since casts need to be changed almost weekly for multiple weeks. This serial casting technique allows the foot to stretch gradually without causing too much pressure in any one area at any one time.
If the foot doesn’t correct with non-surgical techniques, surgery will likely be recommended. If some of the deformity improved with casting, the surgery may be limited to behind the ankle area alone. If, however, the foot remains rigidly deformed, the surgery will be more extensive and typically done just prior to one year of age.
The goal of surgery is to correct the position of the bones within the foot. This will likely require lengthening tendons or ligaments to allow the bones to be moved. The bones are then held in place with pins and a cast. The pins can usually be removed in the office in 4 to 6 weeks. A special shoe or brace may be recommended to try to prevent recurrence of the deformity. Your doctor will likely recommend follow up visits for a few years to see make sure the foot grows well and doesn’t need additional treatment.