
 POSNA.org
POSNA.org
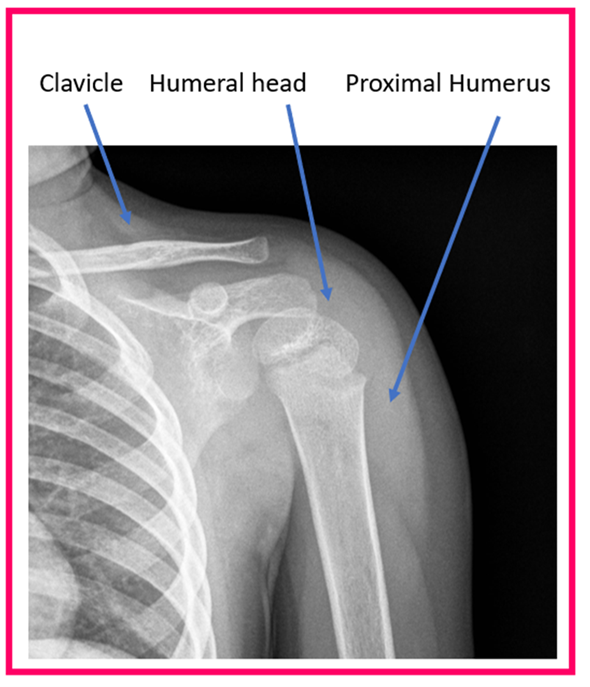 The humerus, or arm bone, is one the major bones in the arm. The humerus bone connects the shoulder joint to the elbow joint. Fractures of the upper part of the humerus bone (proximal humerus) are common in children and adolescents.
The humerus, or arm bone, is one the major bones in the arm. The humerus bone connects the shoulder joint to the elbow joint. Fractures of the upper part of the humerus bone (proximal humerus) are common in children and adolescents.
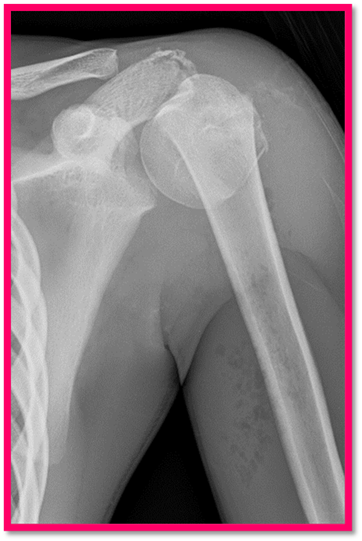 Proximal Humerus Fractures: Break in the top part of the humerus bone, near the shoulder joint. These injuries sometimes can affect the growth plate. This information sheet refers to this type of fracture.
Proximal Humerus Fractures: Break in the top part of the humerus bone, near the shoulder joint. These injuries sometimes can affect the growth plate. This information sheet refers to this type of fracture.
Humeral Shaft Fractures: Break in the middle part of the humerus bone. 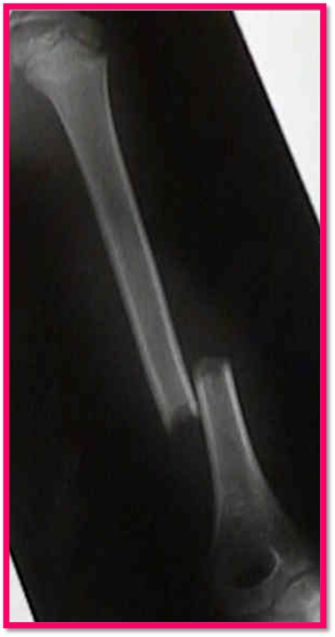
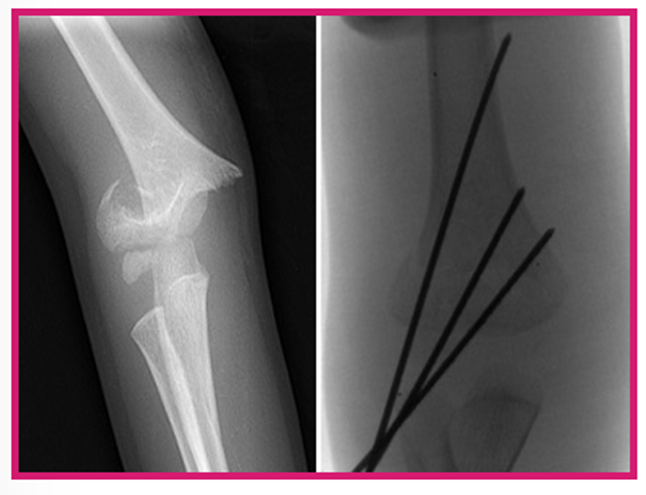
Distal Humerus Fractures: Break in the bottom part of the humerus bone (supracondylar humerus) near the elbow. These injuries are discussed in the elbow fracture information sheet.
Pathologic Proximal Humerus Fracture: Break that occurs through a cyst or tumor in the bone. These injuries may sometimes need specific imaging such as an MRI for diagnosis and often need different forms of treatment than what will not be discussed in this information sheet for proximal humerus fractures.
Little Leaguer’s Shoulder: Injury of the growth plate that happens from chronic, repetitive overuse. This is not a true break in the bone but sometimes treated similar to a break, in that prolonged periods of rest are needed for the growth plate to heal completely.
A swollen and painful arm or shoulder should be checked for a proximal humerus fracture. Children with this injury are unable to use their arm. This injury commonly occurs from blunt trauma such as a fall from standing height on the shoulder, but it can also occur with high-energy trauma, such as a motor vehicle accident or a fall from height. It usually occurs as an isolated injury, but the child should be checked for other injuries if there was a high-energy trauma.
Doctors will check the skin and touch different areas of the shoulder and arm to confirm that the fracture does not extend to the middle part of the bone. He or she will also palpate the bones around the arm including the collarbone, as well as check the nerves and circulation to the arm.
Typically, x-rays will be taken to confirm the diagnosis of a proximal humerus fracture. The x-rays include multiple views to assess the break and confirm the shoulder joint is reduced (not dislocated). Sometimes, additional tests like a CT scan may be needed if the break is complex or in several pieces. An MRI may be considered if the break happens in the setting of a bone cyst or after minor trauma.
Proximal humerus fractures are treated based on the age of the child and alignment of the fracture, or the way the bone pieces sit next to each other. Most proximal humerus fractures in children can be treated with non-surgical treatment, in the form of a sling, a shoulder immobilizer, or sometimes a cast that creates some gentle weight on the arm to align the bones. Periodic follow-up may be needed to ensure healing and the total time of immobilization is usually 4-6 weeks. Between 2-6 weeks after the injury, your provider may allow the child to begin shoulder range of motion. The child will not be allowed to lift objects for the first few weeks, but your doctor may allow some weight-bearing after 6-8 weeks if there is enough evidence of healing on x-ray. Sometimes, fractures heal in a position that is not completely straight. However, some angulation does not affect arm or shoulder function and is therefore acceptable, particularly since and the break continues to “remodel” or straighten as the child grows.
Surgery may be needed if the break is moderate or severe in an older child or if the break extends to the shoulder joint. First, an attempt may be made in the emergency room or in the operating room to manipulate the bones into a better position (referred to as a “closed reduction”), or in more severe cases, an incision may need to be made to align the bones directly (referred to as an “open reduction”). Different types of implants can be used to fix the broken bone, including metal pins/wires, flexible nails/rods, screws, or plates and screws together. A sling is generally still needed, at least in the early weeks after such a surgery, to protect the bone during healing. 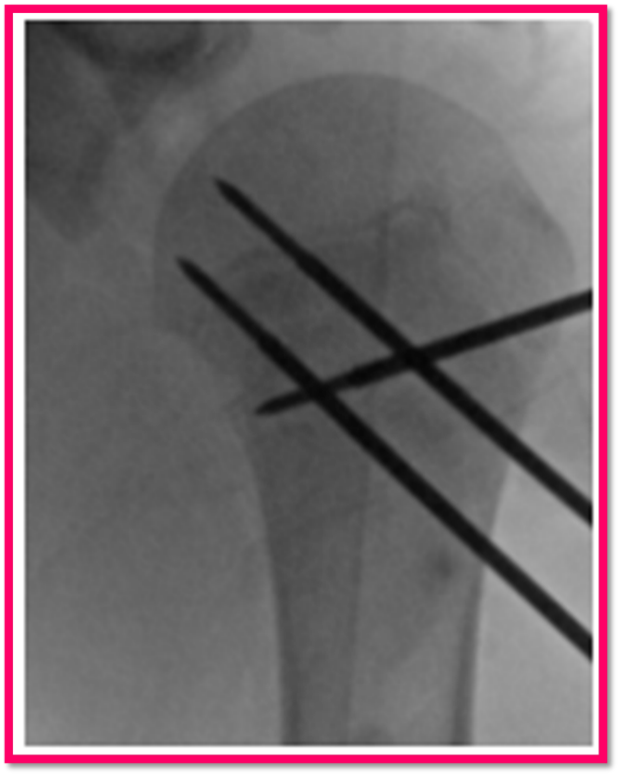
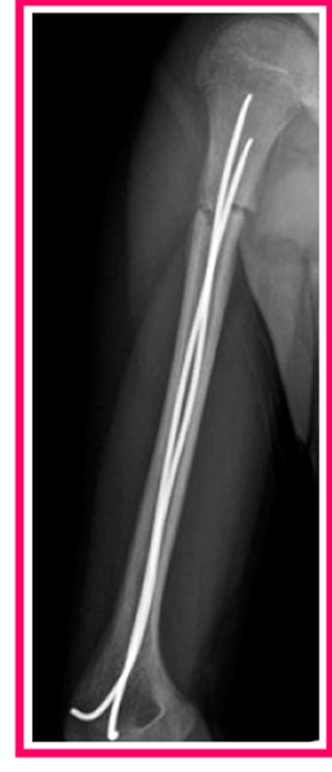
Most children recover from their proximal humerus fracture within a few months. The doctor may monitor your child for a few years to make sure the break undergoes the “remodeling” process, or straightens over time. If your child was treated with an implant, the doctor may recommend removing the implant, either in the clinic, which is done routinely with minimal pain for the child, or in the operating room. Some children will require physical therapy to regain their motion and strength especially after surgery.
Children are not little adults, but like adults, they need expert care. A pediatric orthopaedic surgeon should typically manage these injuries in children in order to decrease the risk of complications and increase the likelihood of a good outcome.
Page QR Code:

If pins or metal implants were used in a surgery for your child’s proximal humerus fracture, the decision to remove implants depends on multiple factors, including patient’s age, injury pattern, activity level, fracture location, and pain from the hardware. Many times, this is a shared decision with your surgeon. If the implants are removed, this typically occurs in one of two scenarios: (1) in the clinic, which is done routinely with minimal pain for the child, or (2) in the operating room as a separate minor procedure.
Fractures may heal as early as six weeks, depending on the severity, but they can take up to several months to heal completely. Return to activities and sports will be determined by your surgeon based on the injury, facture healing, and your child’s age. Return to activities before complete healing can lead to repeat injury.
Most children can return to activity with simple home-based exercises. Older patients, patients returning to high-level sports, and/or patients with a prolonged time for healing may occasionally require formal physical therapy to return to activities.
This is a rare complication for this type of fracture. Your surgeon will see you at regular intervals after your fracture has healed to ensure this is not occurring. If this does occur, there are surgeries that can be done to correct the problem.