Overview
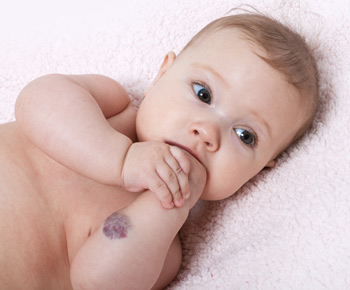
Hemangiomas are benign collections of blood vessels. They are common, especially in infants. They may occur anywhere in the body. If they are in the skin or just below the skin, they are visible as a reddish or bluish discoloration. There may or may not be a bump. Hemangiomas can also occur in the deeper tissues, such as muscle or bone. Hemagiomas are NOT cancer, and it is extremely rare for one to become cancer. Many times hemangiomas do not require treatment, but many patients want them treated if the bump is very discolored and in a very obvious place, such as the face.
We do not know exactly why hemangiomas form. There is no connection between chemicals, radiation, food, medication or activity during pregnancy to cause hemangiomas.
Description
Hemangiomas are arteries and/or veins that multiply more than they should. This collection of blood vessels forms a mass. They are usually painless, red to blue colored lesions. They are usually painless, but superficial lesions may bleed or become sore if bumped or injured.
Infantile hemangiomas are common. They may be present at birth or appear after the first few weeks of life. Usually, these hemangiomas will get bigger quickly in the first year of life and then will start to shrink. It may take many years for the hemangioma to completely disappear. If the hemangioma does not shrink on its own, or if the hemangioma is on a very noticeable place, such as the baby’s face or head, your doctor might recommend treatment.
Hemangiomas may also occur inside muscle and bone. These deep hemangiomas may become painful.
Vascular malformations are different from hemangiomas. Vascular malformations are when clusters of blood vessels develop in arteries, veins, or lymphatic vessels. These are often present at birth and grow slowly with your child. Many of these require treatment.
Doctor Examination
Your doctor will talk to you and your child about his or her medical history as well as any symptoms. He or she will ask about any pain, such as pain with activities or during the night.
Your doctor will ask if there are any masses or lumps, and whether those areas are painful. He or she will feel and inspect the skin and region of the mass.
Studies
X-rays only show bone. They may not show a hemangioma unless there are small areas of calcium inside the hemangioma.
An MRI is often ordered because it shows soft tissues and the hemangioma is easier to see. The MRI may also be done with an angiogram, which is when dye is injected into the vessels.
Treatment
Biopsy
Despite getting X-Rays and an MRI, sometimes the diagnosis of hemangioma cannot be made for sure unless the tissue is examined under a microscope. In order to obtain that tissue, your surgeon will need to biopsy the lesion. For most children, this involves going to the operating room. While your child is completely asleep with anesthesia, your surgeon will take a sample and look at it under the microscope with a pathologist.
Nonsurgical Treatment
Many times, the hemangioma can be observed. Your doctor will want your child to come for regular appointments to monitor any growth or change in size.
Steroids may be used to slow the growth of the mass. This may need to be injected into the hemangioma, or may be taken by mouth.
Compression with stockings and bandages can help decrease swelling but it will not make the hemangioma go away.
Some hemangiomas are candidates for embolization, which is when a substance is injected into the blood vessels to try to close them off. Sclerotherapy is when the injected substance shrinks the vessels. Embolization and sclerotherapy will help to shrink the tumor, so this can be useful before surgery. The hemangioma may regrow its blood supply, though, after embolization or sclerotherapy.
Surgery
If the hemangioma is painful or very large and starting to crowd the normal tissue, your surgeon may recommend an excision. This is when the surgeon removes the hemangioma in the operating room. Even with the best excision, there is a chance that the hemangioma may come back, so your surgeon will want your child to come back for regular appointments after the surgery.
Outcomes
Most infantile hemangiomas will shrink on their own and require no treatment except observation. Other types of hemangiomas may require treatment, especially if associated with pain.
More Information
Condition QR Code:


 POSNA.org
POSNA.org