Description
Charcot Marie Tooth (CMT) is one of several neurological (nerve-related) conditions that are collectively called Hereditary Sensory Motor Neuropathies (HSMN). These are progressive diseases which mean they will get worse over time.HSMN are genetic conditions that are most often passed down from a parent to child. CMT can be passed down two different ways. The most common way is called autosomal dominant inheritance. Autosomal dominant inheritance means that the child of a patient with CMT has a fifty percent chance of inheriting the condition and only needs one gene from one parent. The other way to pass this down is through recessive inheritance. This means for a child to have the condition, both parents must carry the gene, and both need to give the gene to the child.
There are two major types of CMT, but now there are many subtypes of the condition, which have been described due to genetic testing. The severity of the disease can be different in different family members. The disease causes much more involvement with the motor system than the sensory system of the body. It is often symmetrical to some extent, which means there are similar problems on both sides of the body. About 1 in 2,500 to 1 in 5,000 people will get the condition.
Both boys and girls can get CMT at the same rate, but boys have worse symptoms than girls. Girls can often be without symptoms.
Symptoms
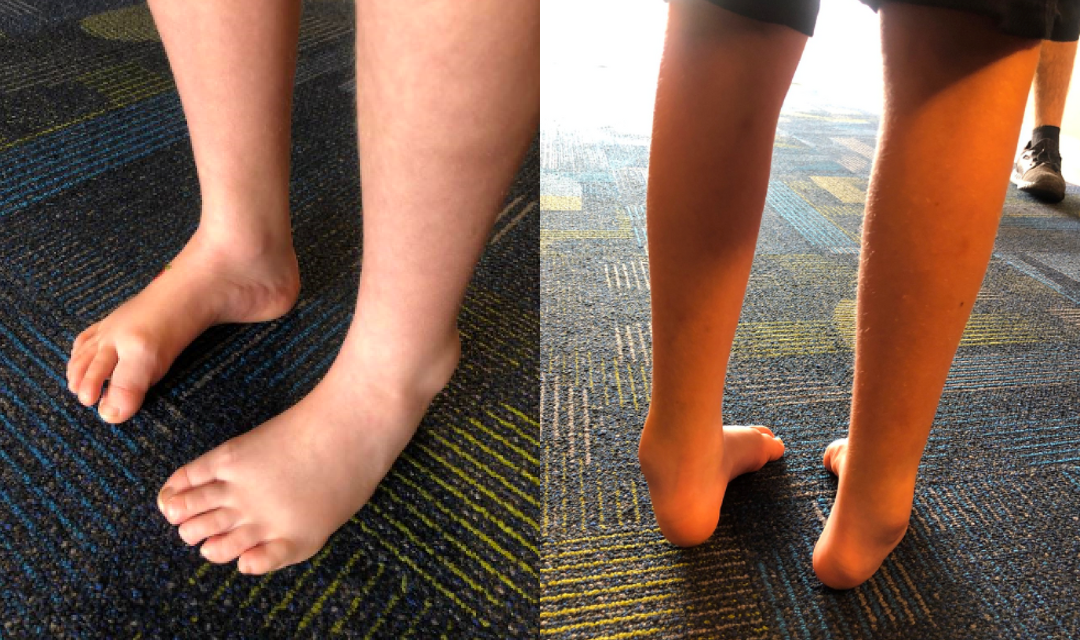
The condition usually becomes evident in the twenties and thirties, but sometimes symptoms can develop sooner. Physical examination is usually normal in children and they usually reach their developmental milestones normally. Over time, weakness and deformity are the two major problems. There is often drop foot present during walking, where the foot slaps the ground because the muscles that hold the foot up during walking have weakened. Certain muscles in the legs may weaken and others do not. When the stronger muscles start overpowering the weaker muscles over time, the feet start to deform and this can become a permanent deformity (Figure 1). There is often a high arch and the heel can slope inward. The foot often inverts or turns inward during walking. The toes may become clawed over time. Most patients will have some atrophy of the leg muscles and some patients will have enough muscle weakness that the patient will be unable to walk.The hands may show atrophy and often the patients will have weakness and inability to hold objects very well. Symptoms with the hands usually start to occur later in life and there is less information on treatment for hand conditions than for the legs.
Hip dysplasia can develop over time in a small percentage of patients and should be treated proactively with reconstruction of the hip. This is often not evident on an exam or any other symptoms from the patient, so the hips should be checked by X-rays in most patients.
Scoliosis can occur in over a third of patients and should be evaluated by an exam and X-rays when deformity is found. Treatment is similar to other types of scoliosis, but bracing has not been effective in preventing progression of CMT-related scoliosis.
More than two-thirds of patients complain of neuropathic pain from this condition. This occurs mostly in the back, feet and legs. Sometimes this pain can be severe enough to require medication.
Diagnosis
This condition can often be evident by the deformities of the feet and the presence of family history. However, a neurologist should be consulted and genetic (chromosome analysis) and nerve testing (EMG) can be performed to confirm which type of CMT the patient has. Most types look fairly similar clinically so genetic testing can be helpful in determining the exact type. Up to 90% of patients can be diagnosed by genetic testing. EMG can be helpful if genetic testing is not conclusive. In a few patients, a nerve biopsy may be necessary to complete the diagnosis.
Treatment
There is no cure for CMT. In the future, genetic treatment may become available. Early bracing can be helpful to keep the foot from slapping and turning inward during gait, and hopefully slow some of the progression of the deformities. Later, after the weakness gets worse or deformity starts in, surgery can be helpful. Tendon transfers and bone surgery to reposition the foot can be helpful. If diagnosed early, some patients will do well with just tendon surgery to balance the foot, but once bone deformity has set in, more extensive bone surgery is often required.
Patient Quality of Life
It is well known that CMT adversely affects the quality of life of the patients that have the condition. Physical, emotional and social aspects of patient’s lives are all affected. Accurate diagnosis, close follow up and different treatments can be helpful in the short term. Surgery is beneficial, but the deformity may return due to the progression of the disease and longer term follow-up is necessary.
More Information
- Orthoinfo - Charcot Marie Tooth Disease
Condition QR Code:




 POSNA.org
POSNA.org